Rhinoseptoplasty
(Rhinoplasty + Septoplasty)
What is rhinoseptoplasty?
Rhinoseptoplasty or septorhinoplasty refers to plastic surgery of the external nose and nasal septum. Rhinoseptoplasty is considered to be one of the most complicated types of plastic surgery, given the high aesthetic value of the nose, its complicated anatomy and the uniqueness of every individual nose. The operation involves realignment of the deformed nasal septum, altering the appearance of the external nose.
Rhinoseptoplasty combines aesthetic rhinoplasty and functional septoplasty into a single whole. The patient can thus avoid undergoing two operations under general anaesthesia completely unnecessarily and all the risks, discomfort and sick leave involved. More severe deformities of the external nose are often associated with deviations of the nasal septum that consequently significantly restrict breathing through the nose. On the other hand, mobilisation, reposition or reconstruction of the nasal septum is an essential prerequisite for the successful correction of deformities of the external nose. Where indicated, rhinoseptoplasty is followed by laser or radiofrequency reduction of the volume of the lower conchae (mucotomy, turbinoplasty), which may further improve nasal patency.
When is rhinoseptoplasty recommended?
Rhinoseptoplasty is indicated in patients suffering from a combination of an aesthetic deformity of the nose (nasal scoliosis, aquiline nose, saddle nose etc.) and deviation of the nasal septum. These disorders are either congenital or acquired (e.g. after injury, including birth injury). The nasal septum is not located in the midline in approximately 75% of Caucasians. However, only part of these deformities is associated with functional problems. Unfortunately, we are seeing more and more patients whose external nose deformities are the result of previous surgery during which the aesthetic aspect of the surgical procedure took precedence over the functional aspect.
Rhinoseptoplasty may be performed even in patients who had sniffed drugs such as cocaine in the past. These patients often suffer from a perforated nasal septum and in the most serious of cases there may be destruction of the cartilage skeleton of the external nose, of the external wall of the nose as well as of the palate. Reconstruction of the nasal skeleton may be attempted only once the patient stops taking drugs, the inflammatory changes are treated and the patient´s condition stabilises. In most cases, cartilage or composite (combined with skin) grafts taken from the patient´s auricles or ribs have to be used. It is naturally necessary to use skin flaps to renew normal mucosa.
The recommendation to undergo this type of surgery is given either by an outpatient ENT specialist or a general practitioner. You may come for a non-binding consultation even without any such recommendation.
What are the consequences of deviations of the nose?
Deviation of the nasal septum first and foremost leads to a unilateral or bilateral disorder of nasal patency. This is then associated with a disruption of other physiological functions of the nose such as moistening, warming and cleansing of the inhaled air. The flow of air through the sites of pathological narrowing leads to changes in the nasal mucosa and stagnation of nasal secretions, which may be associated with the formation of crusts and a sensation of dryness of the nose. In some cases, patients complain of recurrent headache or tension in the head or of olfactory disorders. The switch to breathing through the mouth, which is natural only in the short-term under specific conditions such as on exertion, affects negatively the pharynx and lower respiratory tract. This may then lead to impairment of sleep quality and thus of overall performance and productivity.
At what age is it suitable to undergo septorhinoplasty?
Ideally, this surgical procedure should be performed once growth has stopped in adolescence. This roughly corresponds to the age of 16-18 years in women and 18-20 years in men. In indicated cases (severe deformities of the nasal septum, acute trauma, haematoma or abscess of the nasal septum), it is possible to operate in childhood. However, certain rules must be followed and a maximally conservative approach should be preferred. If it is absolutely necessary to remove any cartilage, the removed tissue must be re-implanted or replaced by a suitable graft (ear or rib cartilage). Otherwise, there is a risk of disrupting the development of the external nose and mid-line structures of the face.
The upper age limit has increased significantly over the past few years and surgery involving sixty-year old or older patients is no longer an exception. The so-called „aging nose“ is becoming an independent chapter in both specialist journals and symposia. Again, in such cases, the indication of such surgery must be considered carefully, taking into account its benefits and possible risks.
What does the operation involve?
This operation is usually performed under general anaesthesia. Once sedated, the patient is intubated using an endotracheal tube. Then, the nasal septum and skeleton of the external nose are modelled using special instruments. Two techniques are used. The closed technique involves surgical incisions only in the nasal vestibule and on the nasal septum inside the nasal cavity. The open technique necessitates a small incision of the nasal columella (the fleshy external end of the nasal septum between the nostrils). The small scar is in a majority of cases aesthetically inconspicuous. The popularity of the open technique has increased over the past 20 years, as it ensures a significantly better overview and access to all anatomical structures and facilitates complicated procedures and more precise reconstruction.
Finally, intra-nasal splints are affixed to the nasal septum. These ensure its stabilisation during the first days after surgery. A nasal tamponade is then carefully inserted into the nasal cavity and an external splint (gypsum, metal, plastic) is placed on the nose. This usually remains in place for 10-14 days. The surgical procedure lasts 1-3 hours, depending on the extent of the nasal skeleton deformity. The patient is then transferred to the post-operative room, where his/her vital functions are monitored for 2-4 hours. After longer and more complicated procedures, patients may be hospitalised at the clinic overnight.
What can you expect after surgery?
Once healing is complete, nasal patency and the appearance of the nose should improve. The first two days after surgery are the most difficult for the patient, as the nasal cavity is filled with the tamponade and breathing is possible only through the mouth. Even once the tampons are removed, breathing through the nose remains restricted because of swelling and the presence of mucus and often some blood. Swelling of the eyelids and bruises in the area of the nose that disappear in most patients within two weeks from surgery occur practically always. The nose should be rinsed with saline solutions and cleansed carefully.
The first check-up should take place 2-3 days after surgery. Another check-up is usually scheduled 1-2 weeks after surgery. The patient usually remains at home for two to three weeks until his/her condition has stabilised. Patients may return to work after this period. The duration of sick leave depends on the character of the patient´s work. Longer sick leave should be expected in the case of occupations involving physical exertion, a dusty environment or contact with chemical substances. In all cases, physical exertion should be gradually increased and not exaggerated.
After what time can you evaluate the aesthetic and functional effects of rhinoseptoplasty?
The aesthetic effect can be reliably assessed only after complete healing, which may take up to several months. Post-surgical changes involving the nasal skeleton may be observed in some patients even after several years. It is important to keep in mind that healing after such surgery cannot be influenced in any fundamental way and even perfectly executed surgery may be associated with both early (bleeding, swelling, inflammation, necrosis etc.) and late complications (perforation of the nasal septum, re-deviation of the nose, decline of the bridge, irregularities of the bridge, deformities of the tip etc.). Potential re-operations should be performed in a vast majority of cases as soon as possible after the initial surgery, ranging from several months to one year, thus guaranteeing complete healing of the operated structures.
We always approach nasal deformities complexly. The main goal of all surgery is to combine the functional and aesthetic components of the surgical procedure into one whole (rhinoseptoplasty) and create a correctly functioning nose of normal shape. We never give precedence to the aesthetic result over renewal of correct functioning of the nose.
Our surgeons

prim. MUDr. Radim Kaňa, Ph.D.
The Head of the ENT Dept. of the General Teaching Hospital in Prague has been attending courses of septorhinoplasty all over the world for more than 15 years. During his career, he has performed more than 3500 surgeries of the nose, of which about 1000 involved rhinoseptoplasty. He ranks among the best in his field in the Czech Republic.

prim. MUDr. Tomáš Fořt
The Founder and Head of FortMedica specialises in surgical procedures involving coblation plasma technology, but he frequently performs septoplasty and has also taken completed several courses of septo- and rhinoplasty. He is the guarantor of quality of all provided services at all FortMedica clinics in Prague.
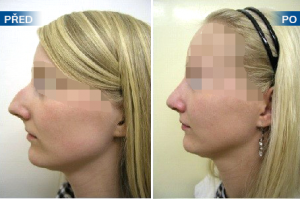
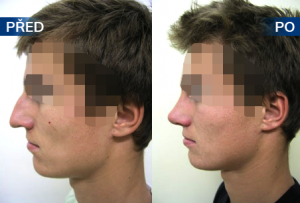
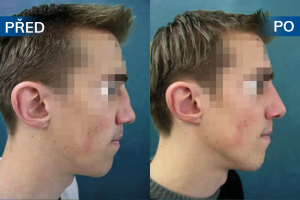
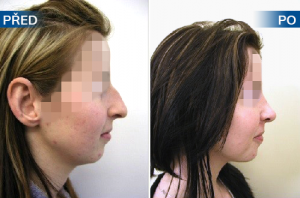
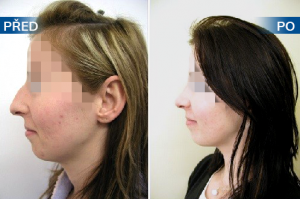
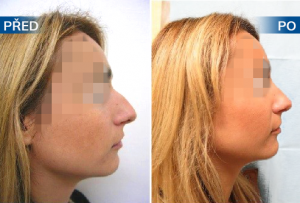
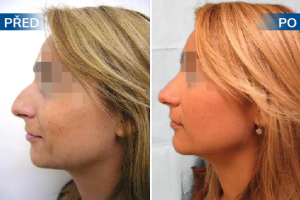
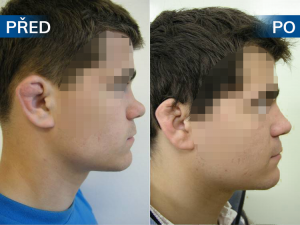
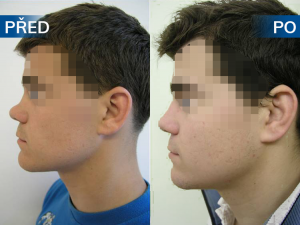
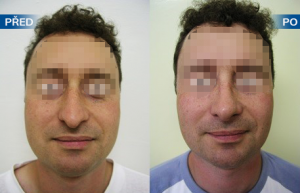
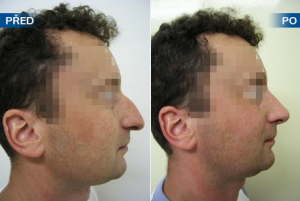
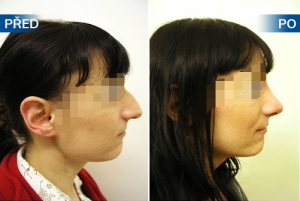
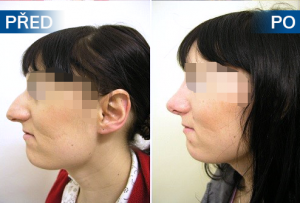
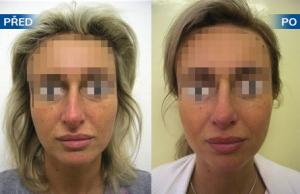
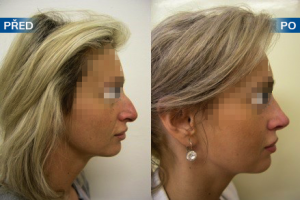
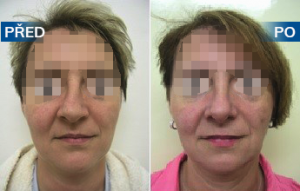
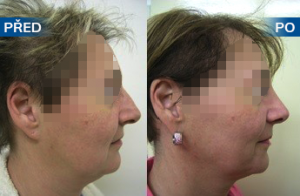
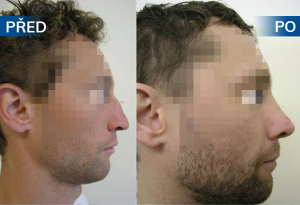
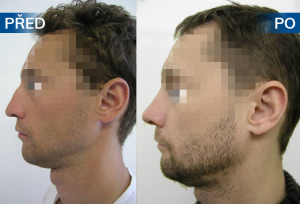
Photo gallery of surgical procedures
Patient testimonials
How can you make an appointment?
Rhinoseptoplasty is performed at our branch in Modřany. The patient first undergoes a pre-operative examination during which he/she consults the suitability of the given procedure and potential options with the physician. Please call for an appointment: +420 720 028 820.
The operation usually costs between 25 000 – 45 000 CZK depending on the duration and complexity of the procedure. The exact price is set following the personal consultation of the surgeon. This consultation is free of charge for clients insured by Czech health insurance companies.
We recommend that you also refer to the section “Documents”, where you will find all the documents required before the operation.
Contact us
In case of any other questions regarding surgical procedures you can contact us through this contact form, call us at +420 720 028 820 or you can visit us personally at the doctor’s office in Modřany.